
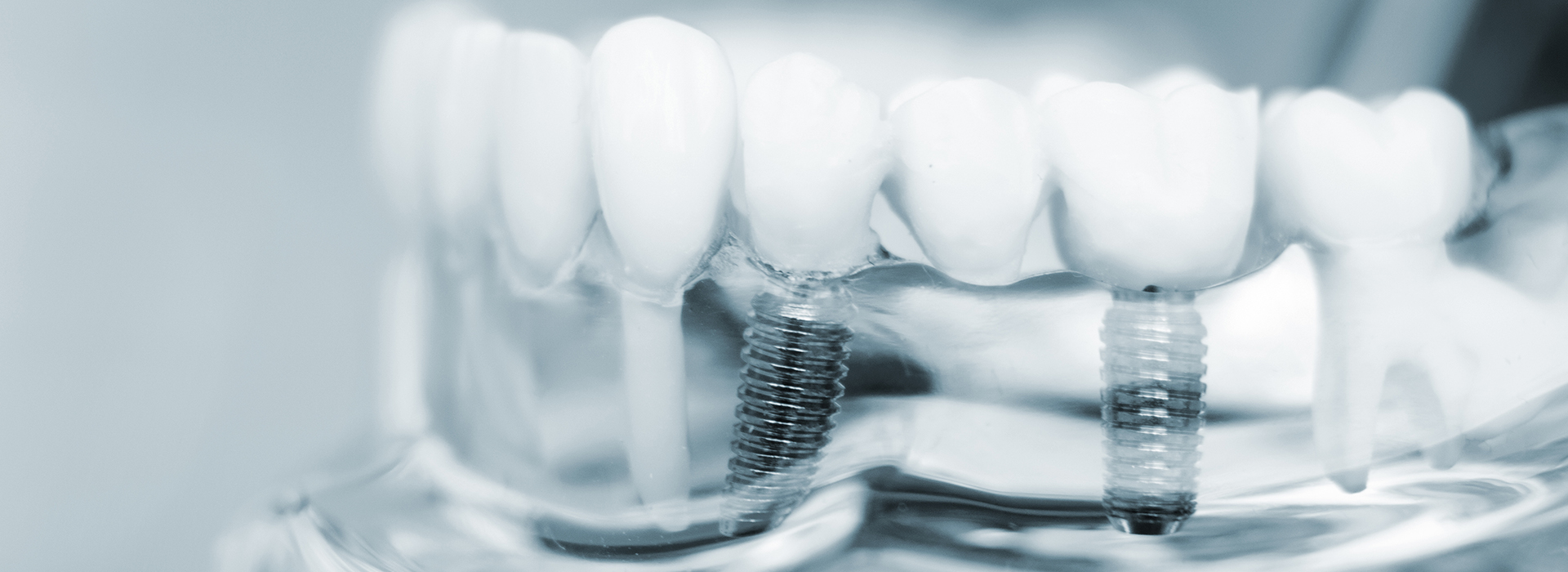

Tooth loss affects people across all ages and lifestyles, but the impact is more than cosmetic. Missing teeth can change how you chew, speak, and how your face appears over time. Our approach focuses on restoring reliable function and a natural appearance so patients can return to daily life without hesitation.
When tooth replacement is planned with precision, the results are durable and feel like a real tooth. Implants recreate the missing root structure and give prosthetic teeth a stable foundation—so you can eat your favorites, laugh openly, and maintain the natural contours of your face.
At the office of The Prosthodontic Center of Beverly Hills, we combine advanced imaging, implant systems, and prosthetic skill to craft predictable outcomes. Treatment is tailored to each patient’s anatomy, lifestyle, and goals so the solution we recommend fits both form and function.

Dental implants are designed to integrate with the jawbone and support crowns, bridges, or full-arch restorations. Because they replace the root as well as the visible tooth, implants preserve bone and avoid the need to alter neighboring teeth the way a conventional bridge might.
Unlike removable dentures, implant-supported restorations resist movement and provide a secure bite. This stability improves chewing efficiency, reduces sore spots, and eliminates the need for adhesives—in turn supporting better nutrition and quality of life.
Implants are also adaptable: a single implant can replace one missing tooth, while several implants can support multiple teeth or an entire arch. This versatility makes them a strong option for many clinical situations where long-term performance and comfort are priorities.
Implants are made from biocompatible materials designed to fuse with bone in a process called osseointegration. After placement, the bone gradually grows around the implant, creating a stable interface that supports the visible restoration.
The timeline for integration depends on the individual, the implant site, and whether any preparatory procedures (like grafting) were required. In many cases, a provisional prosthesis can be provided during healing so appearance and basic function are preserved while the implant bonds with the bone.
Throughout treatment, we emphasize gentle tissue management and precise implant positioning. This attention to detail helps minimize complications and supports lasting aesthetic and functional results.
Beyond appearance, implants help maintain the health of the jaw by delivering the mechanical stimulation bone needs to retain volume and density. This biological benefit helps preserve facial structure and reduces the gradual changes that follow tooth loss.
Implant-supported restorations also simplify home care and long-term maintenance: they’re cleaned much like natural teeth and, with routine dental visits, can remain a dependable part of your mouth for many years. Their resistance to decay and structural stability make them a practical, long-lasting option.
Because implants do not require altering adjacent healthy teeth, they represent a conservative solution for replacing missing teeth. In many situations, implants allow us to restore smiles while preserving as much of the natural dentition as possible.
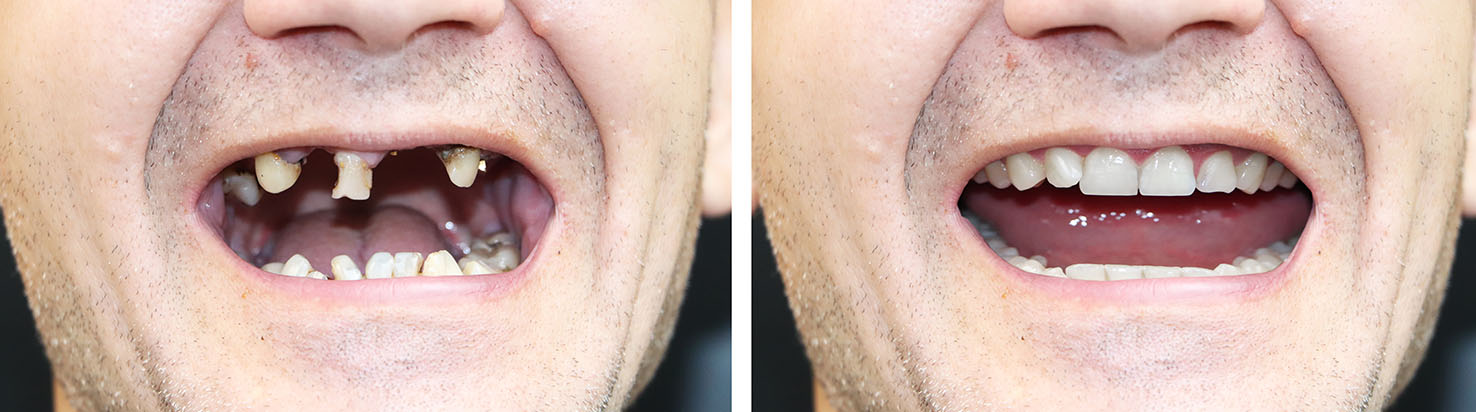
Determining candidacy involves a careful review of your health history, oral condition, and treatment goals. We evaluate bone quality and quantity, gum health, bite relationships, and any medical factors that might affect healing. Smoking, certain medications, and systemic conditions can be considerations, but many situations can be managed successfully with proper planning.
Our evaluation uses modern imaging and a thorough clinical exam to map the sites for implants and plan restorations that align with your facial features and functional needs. We emphasize clear communication so you understand the sequence of care and what to expect at each visit.
Every recommendation is personalized. If implants are not the ideal option right away, we’ll outline alternative paths or preparatory procedures—such as bone grafting—that can help make implant treatment possible in the future.
Implant placement is delivered with attention to comfort and safety. The surgical phase is generally outpatient and tailored to the complexity of your case. Local anesthesia is standard, and sedation options are available for patients who prefer additional relaxation during procedures.
After implant placement, a period of healing is needed for osseointegration. During this time, we monitor progress and provide guidance on diet, oral hygiene, and activity to support predictable healing. When integration is complete, the restorative phase begins—crafting replacement teeth that match form, shade, and bite.
Careful planning, precise surgical execution, and collaboration between the surgical and prosthetic phases all contribute to outcomes that are comfortable, functional, and long-lasting. We’ll keep you informed throughout each step so you can make confident decisions about your care.
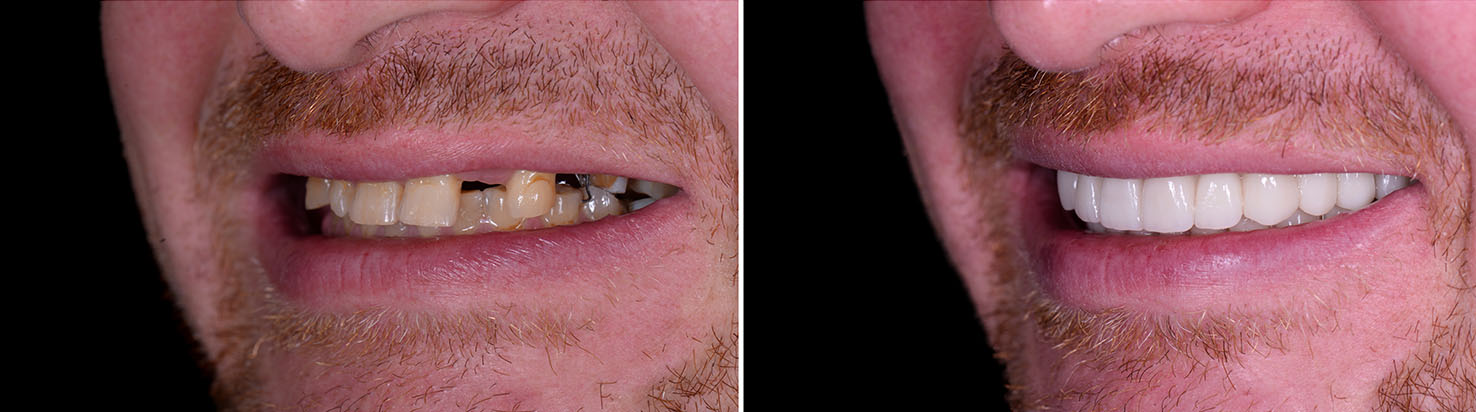
Successful implant placement requires adequate bone to support the implant. If tooth loss, infection, or anatomy has reduced bone volume, grafting procedures can rebuild the ridge to provide a stable foundation. Grafts can be placed at the time of extraction, before implant placement, or in combination with implant surgery depending on the clinical situation.
Bone grafting uses safe, well-established materials and techniques to encourage the body’s natural regenerative processes. While grafting adds an additional step to treatment, it often enables predictable implant placement in areas that would otherwise be unsuitable.
Replacing missing teeth with implants restores more than a smile—it restores function, comfort, and the confidence to enjoy life fully. Our practice blends surgical expertise and custom prosthetic design to achieve outcomes that look natural and perform reliably.
If you’d like to learn more about implant dentistry or discuss whether implant treatment is appropriate for your needs, contact our office for more information. We’re here to answer your questions and help you take the next step toward a complete, healthy smile.
Implant dentistry replaces missing teeth by placing biocompatible posts into the jawbone that act as artificial roots. These posts support crowns, bridges, or full-arch prostheses to restore chewing, speech, and facial contours. Because implants recreate the root structure, they offer a stable foundation that closely mimics natural tooth function.
Implants are typically made from titanium or titanium alloys and integrate with bone through a process called osseointegration. Treatment includes careful surgical placement followed by a restorative phase in which custom prosthetic teeth are attached. At the office of The Prosthodontic Center of Beverly Hills we combine advanced imaging, surgical planning, and prosthetic expertise to design restorations that match form and function.
Unlike traditional bridges, which rely on adjacent teeth for support, implants replace the root as well as the crown and therefore help preserve surrounding tooth structure. Compared with removable dentures, implant-supported restorations resist movement and provide improved chewing efficiency and comfort. The increased stability often reduces sore spots and the need for adhesives.
Implants can be used to support a single crown, an implant-retained bridge, or a full-arch restoration depending on the pattern of tooth loss and patient needs. Because they stimulate bone, implants help maintain jaw volume and facial contours that otherwise diminish over time after tooth loss. This combination of function and biology makes implants a durable and conservative choice in many clinical situations.
Candidacy for implants is based on a comprehensive review of your medical history, oral health, and specific anatomic factors such as bone volume and gum condition. Good overall health and healthy soft tissues around the future implant site increase the likelihood of predictable healing, but many systemic conditions can be managed with appropriate planning. Smoking, uncontrolled diabetes, or certain medications may influence timing or require additional precautions rather than automatically disqualifying a patient.
Our evaluation uses clinical examination and modern imaging to measure bone quality and map implant positions before any surgical steps are taken. When bone or tissue is insufficient, preparatory procedures such as grafting or soft-tissue augmentation can often create the foundation needed for successful implant placement. Every treatment plan is individualized to align with the patient’s goals, anatomy, and long-term oral health needs.
The implant treatment process begins with a consultation and diagnostic phase that includes X-rays or cone-beam computed tomography to plan implant positions precisely. Once planning is complete, the surgical stage places the implant into the jawbone under local anesthesia, and sedation options may be offered for patient comfort. Simple cases may involve a single implant and crown, while more complex reconstructions require staged procedures and coordination between surgical and restorative care.
After implant placement, a healing period allows bone to integrate with the implant before the final prosthetic is attached, and provisional restorations can maintain appearance and basic function during this time. The restorative phase involves designing and fitting crowns, bridges, or full-arch prostheses to achieve proper bite, shade, and esthetics. Throughout treatment, regular follow-up visits ensure proper healing and timely progression to the next phase.
Healing and osseointegration timelines vary with the patient and the implant site, but many cases require several months for stable bone integration. Factors such as bone density, the need for grafting, and the location in the mouth can lengthen or shorten this period. Practitioners monitor healing clinically and radiographically to determine when it is appropriate to begin the restorative phase.
In some protocols, immediate provisional teeth are placed at the time of surgery to preserve esthetics and function while osseointegration progresses. Other approaches delay loading until integration is confirmed to reduce the risk of micromovement and implant failure. Your care team will recommend the timing that balances healing biology with your functional and cosmetic needs.
Bone grafting rebuilds deficient jawbone to provide a stable foundation for implants when natural bone volume is inadequate. Grafting materials may include autograft, allograft, xenograft, or synthetic substitutes chosen to encourage the body’s regenerative response. The choice of material and timing depends on the extent of loss and the planned implant approach.
Grafts can be placed at extraction, before implant surgery, or simultaneously with implant placement depending on the situation and the clinician’s assessment. Although grafting adds an additional phase to treatment, it frequently enables implant therapy in areas that would otherwise be unsuitable. Your treatment plan will describe expected healing times and follow-up needed to assess graft maturation before proceeding with final restorations.
Single-tooth implants restore an individual missing tooth without altering adjacent teeth and are finished with a custom crown that matches the surrounding dentition. When multiple adjacent teeth are missing, implant-supported bridges can replace all missing crowns using fewer implants than individual replacements. For patients missing a full arch, fixed implant-supported prostheses recreate a non-removable set of teeth that restores function and eliminates the need for conventional dentures.
Removable implant-retained overdentures offer improved retention and comfort while allowing removal for home care, combining the benefits of stability and maintainability. Each restoration is designed to address esthetic goals, bite relationships, and long-term maintenance requirements. The restorative design is selected to match the patient’s preferences, anatomy, and lifestyle expectations.
As with any surgical procedure, dental implant therapy carries risks such as infection, delayed healing, or failure of the implant to integrate with bone. Less common complications include nerve irritation or sinus involvement when implants are placed near these structures. Careful planning and imaging reduce these risks by identifying anatomic limits and optimizing implant size and position.
When complications occur, they are managed with prompt clinical intervention that may include local treatment, antibiotics, modification of the prosthesis, or revision surgery when necessary. Long-term success also depends on patient adherence to oral hygiene and regular maintenance visits to detect and treat problems early. Open communication with your care team allows tailored strategies to mitigate risk and address concerns as they arise.
Daily home care for implants mirrors good natural-tooth hygiene and includes thorough brushing and interdental cleaning to remove plaque around implant restorations. Specialized tools such as floss threaders, interdental brushes, and water irrigators can help clean beneath bridges and around implant-supported prostheses. Avoiding hard or abrasive habits and addressing parafunctional forces with protective appliances reduces mechanical stress on restorations.
Professional maintenance appointments are essential to monitor tissue health, check for signs of inflammation, and perform targeted cleaning around implant components. Your clinician may recommend a customized recall schedule based on your risk factors and the type of restoration in place. With attentive home care and professional follow-up, implants can remain a stable, long-term part of your oral health plan.
Before implant surgery you will receive specific preoperative instructions that may address medication management, instructions for fasting if sedation is planned, and recommendations for smoking cessation to support healing. It is important to share a complete medical history and a current list of medications so the team can assess any factors that affect anesthesia and healing. You may be advised to arrange transportation and limit strenuous activity for a short period after the procedure.
On the day of surgery, bring any required forms and wear comfortable clothing, and expect clear post-operative instructions and scheduled follow-up to monitor healing. If you have questions or experience unexpected symptoms, contact the office promptly to allow timely evaluation and care. The Prosthodontic Center of Beverly Hills prioritizes clear communication and coordinated surgical and restorative care to help patients move through each stage with confidence.